A vp shunt is basically an automated external device that performs a V2 shunt in patients with severe cerebellar atrioventricular conduction (CAC) disease.
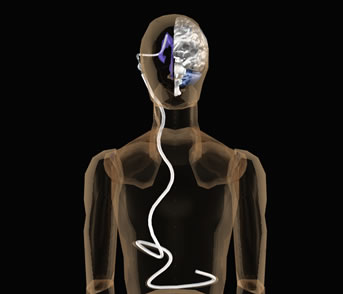
A V2 shunt is a device that regulates the pressure and flow of cerebrospinal fluids from the ventricles to the interventricular septum. As the volume of cerebrospinal fluids in the cerebrum increases, the open one-way channel in the shunt closes and the excess fluid flows into the posterior cavity. This procedure is used for controlling the amount of cerebellar cerebrospuncular fluid (CSF) that is pumped into the cerebrum in patients with CAC and other diseases that affect the flow of cerebrum-cerebellar fluid interaction.
A VP shunt is used by many physicians to reduce the pressure in the brain and to provide relief to patients suffering from CAC. The V2 shunt also has the capability to reduce the size of tumors that are causing the symptoms of CAC. The procedure works by regulating the flow and the pressure in the cerebrum.
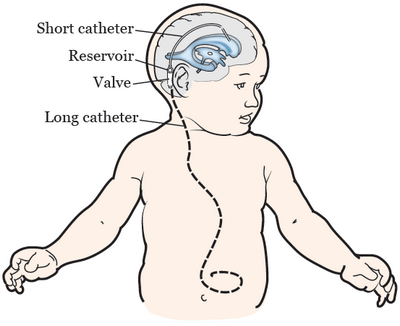
This in turn, allows the blood to flow easier into the ventricles and to prevent them from narrowing down. When the blood does not have to travel through the arteries as fast, this reduces the amount of stress that is placed on the nerve fibers in the cerebrum.
One of the main reasons why VP shunts are used in CAC treatment is that they provide better control over the amount of fluids that are pumped in and out of the cerebrum. One of the most common and serious side effects of surgery is fluid build-up in the cerebrum and in the interventricular septum. This fluid buildup is caused by the increased amount of fluid in the arteries that is not being transported into the cerebrum. This increase in pressure can result in a stroke or a potentially dangerous condition called pericardial effusion.
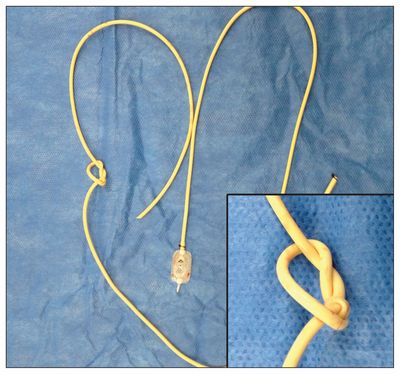
It can also result in significant damage to the nerves in the cerebrum, if the water that has gathered in the cerebrum does not drain out into the interventricular septum. This is a risk that is significantly reduced in the case of VP shunts.
Patients who are suffering from CAC or who need to use this procedure to treat the symptoms of the disease often have a variety of symptoms to deal with. A patient may experience either focal neurologic deficits, which can include problems with movement, balance and reflexes; seizures; headaches; severe headaches; or even paralysis. Some of these symptoms can become so severe that it is difficult to keep up with them. For this reason, it is imperative that doctors know when these symptoms are presenting so that they can make a plan to get the treatment right before they become severe.
Many doctors use a VP shunting procedure to help control the fluid buildup in the interventricular septum so that the pressure of the cerebrospinal fluid will be increased in the brain.
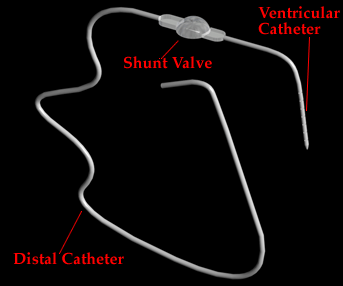
This increased pressure will allow the fluid to drain more easily into the posterior cavity. This allows the brain to have an easier time in moving fluid from the interventricular septum to the cerebrum.
There are a variety of V2 shunt types and all of them have their pros and cons. They include:
Ultrasound guided shunt: The ultrasound guided shunt is very similar to a traditional shunt but instead of measuring the amount of fluid going into and out of the ventricle, a thin probe is inserted into the ventricle and guided through a small hole into the cerebrospinal fluid. In this type of shunt, a digital camera is used to monitor the fluid flow in the ventricle.
Digital shunt: An ultrasonic shunt involves a radio transmitter that transmits sound waves through radio waves and is located within the skull. This sends radio waves that are received by the probe that measures the fluid pressure in the interventricular septum and cerebrum.
If you are considering VP shunts for your treatment then it is important that you discuss the options with your doctor. If you feel that you are going to need the procedure more than once then you might want to consider one of the other shunt types.